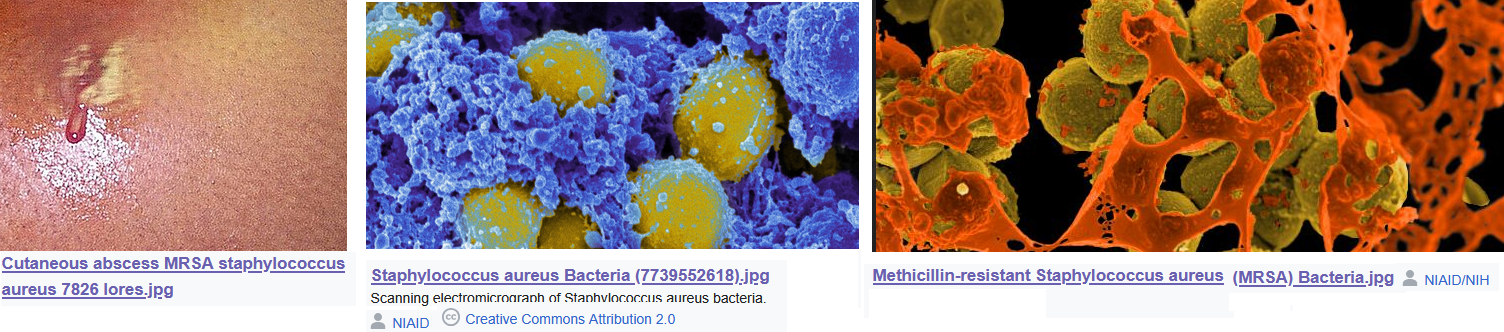
Staphylococcus aureus is a factor in atopic dermatitis. This post is a continuation of killing faculatative anaerobes with very low frequency PEMF. This post makes the case the PEMF can kill Staph aureus in in vitro systems and gives an introduction to atopic dermatitis. The sister post, Staph aureus metabolism, deep dives into possible antenna for PEMF in Staph aureus. The featured image is composed of public domain scanning electron microscope images of Staph aureus on cellular debris. The conclusion is that never mind the metabolism, maybe PEMF has another beneficial mechanisms.
Treatments for Staph aureus atopic dermatitis
Of the many very excellent reviews, Schachner 2024 is probably best for the purpose of this post.
- The overall skin microbiome is important.
- Staphylococcus aureus is the main culprit.
- Long-term antibiotic therapy has social consequences in terms of antibiotic resistance.
- Some peer reviewed publications suggest dilute bleach baths are effective.
- The review cited references suggesting that dilute bleach baths improve the microbiome as well.
- Other Schachner 2024 referenced studies showed no improvement over normal water baths.
- topical microbiome transplantation was cited as an option.
- S. aureus targeting phage endolysin could be an option. Phage are viruses that infect bacteria.
- Zabalafin is a hydrogel with multiple mechanisms of action that the Schachner 2024
Itch and atopic dermatitis
Gallo and Horswill and 2024 address the role of S aureus in childhood atopic dermatitis in a cartoon. PEMF practitioners claim that PEMF reduces inflammation by inhibiting adenosine pathways. This concept is addressed in the PEMF for inflammation post. The Gallo and Horswill 2024 cartoon, makes note of the adenosine pathways in itch and inflammation indirectly via the “purirepctor.” Purinergic receptors are activated by adenosine, adenosine diphosphate, adenosine triphosphate (ATP)… When a cell is killed by Staph aureus, it releases ATP and ADP. This alerts the body that there has been an attack. My post presents the hypothesis that the pulsed magnetic fields just get charged particles moving via Faraday’s Law of Induction. Once the message of the attack has been sent, it may help to shut off the signal less the sdtatus become chronic.
S. aureus produces several toxins, such as PSMs, phenol soluble modulins, which are amphiphathic helices regulated by the agr accessory gene regulator system. How might PEMF affect these molecules if their charges can respond to a magnetic field?
Very low frequency PEMF inhibits Staph aureus in table form
One of the frustrating things about these very promising studies is that they show promise but are not performed under conditions that resemble those in encountered in an actual patient. The authors use standard microbiological media, but do the ingredients change the proteins that the bug expresses? With that caveat, these are some nice examples of promising studies.
| medium | O2 | time | frequency | magnetic field | outcome | ref |
|---|---|---|---|---|---|---|
| Columbia 5% sheep blood broth | room | 37o C for 24h | 0-50 Hz | 0.5-10 mT | 5 mT, 20 Hz 29.2% ↓ CFU (P = 0.0376) | Obermeier 2009 |
| TY broth tryptone yeast | room | 25oC 24 min | 50Hz | 7.1 mT | 20% ↓ CFU p<0.05 | Fojt 2004 |
| Mueller-Hinton broth, protein rich | room | 37o C for 24 h | 20 Hz | 5 mT | PEMF + antibiotic 32.4% of gentamicin alone p=0.0002 | Matl 2011 |
| MHB, in Eppendorf tube | ? | 25oC 1-6hr | 20, 40, 50 | 2 & 4 mT | 6 hr, 4 mT, 20 Hz best. | Bayır 2015 |
There is so much uncertainty as to whether or not these promising results will translate into an infection shown in the left hand side of the featured image. Going into Staph aureus is not the purpose of this post. Perhaps we need to get a mental image of the bugs sitting in cellular debris.
Another mechanism ?
Biohackers use PEMF to clear out inflamed regions. The concept that a moving magnetic field moving charged particles has already been addressed in PEMF and inflammation. Can pulsed magnetic fields break up interactions of bacteria with cellular debris as in the featured images?
References
- Bayır E, Bilgi E, Şendemir-Ürkmez A, Hameş-Kocabaş EE. (2015) The effects of different intensities, frequencies and exposure times of extremely low-frequency electromagnetic fields on the growth of Staphylococcus aureus and Escherichia coli O157:H7. Electromagn Biol Med. 2015 Mar;34(1):14-8. Sci-Hub free paper
- Costa FG, Mills KB, Crosby HA, Horswill AR. (2024) The Staphylococcus aureus regulatory program in a human skin-like environment. mBio. 2024 May 8;15(5):e0045324. PMC free paper
- Fojt, L., Stra ˇsa´ k, L., Vetterl, V., et al. (2004). Comparison of the low-frequency magnetic field effects on bacteria Escherichia coli, Leclercia adecarboxylata and Staphylococcus aureus. Bioelectrochemistry, 63:337–341. Sci-Hub free paper
- Gallo RL, Horswill AR. Staphylococcus aureus: The Bug Behind the Itch in Atopic Dermatitis. J Invest Dermatol. 2024 May;144(5):950-953. free paper.
- Matl FD, Obermeier A, Zlotnyk J, Friess W, Stemberger A, Burgkart R. (2011) Augmentation of antibiotic activity by low-frequency electric and electromagnetic fields examining Staphylococcus aureus in broth media. Bioelectromagnetics. Jul;32(5):367-77. Sci-Hub free paper
- Obermeier A, Matl FD, Friess W, Stemberger A. Growth inhibition of Staphylococcus aureus induced by low-frequency electric and electromagnetic fields. Bioelectromagnetics. 2009 May;30(4):270-9. Sci-Hub free paper
- Schachner LA, Andriessen A, Gonzalez ME, Lal K, Hebert AA, Eichenfield LF, Lio P. A Consensus on Staphylococcus aureus Exacerbated Atopic Dermatitis and the Need for a Novel Treatment. J Drugs Dermatol. 2024 Oct 1;23(10):825-832. free paper
Leave a Reply